Lift Slings: Selecting and Using Them Safely in Patient Handling and Mobility
Lifts protect caregivers and patients alike by reducing exertion required to move patients from point A to point B. Read on for key considerations in selecting and training on lift slings across units and organizations. Listen to the full on-demand webinar to earn one contact hour.
Patient lifts, both powered and non-powered, are essential to safe patient handling and mobility. By facilitating movement of patients to necessary places and positions, they can dramatically reduce risk of injury to both patients and healthcare workers. However, lifts and slings also introduce new considerations and risks due to a variety of factors. The U.S. Food & Drug Administration (FDA) Manufacturer and User Facility Device Experience (MAUDE) database offers a look at adverse events related to patient lifts and slings, and their causes. Sling and hanger bar incompatibility, worn or damaged sling materials, and use of the wrong sling size or type are just a few of the errors and oversights that led to instances of injury and, in some cases, even death.
Of course, choosing slings and ensuring they’re properly maintained and utilized is easier said than done. Sling selection is complicated by the matter of compatibility. No sling is suitable for use with all patient lifts. Meanwhile, some manufacturers offer slings exclusively; others only sell lifts. These moving parts can cause confusion for healthcare organizations when selecting and procuring slings and for healthcare professionals tasked with using them.
Below, we’ll outline key factors in sling selection as well as maintenance and training. But first, a look at regulating bodies overseeing patient sling safety and compliance.
LIFT & SLING GOVERNANCE
Oversight of lifts and slings has come a long way in the past two decades. The International Organization for Standardization (ISO), an independent, non-governmental entity, began overseeing patient lifts in 2006 with the adoption of ISO 10535. Domestically, the FDA, which categorizes lifts and slings as medical devices, recognizes ISO 10535 as the consensus standard, and therefore the minimum standard for U.S. lift manufacturers. ISO 10535 was dramatically updated and expanded in 2021, enhancing sling design and testing requirements as well as communication requirements for manufacturers regarding approved combinations of lifts, hanger bars, and slings. Per FDA best practices outlined on its General Hospital Device and Supplies webpage, any sling must be approved for use by the patient lift manufacturer. To be clear: Slings and lifts do not necessarily need to originate from the same manufacturer. Still, the need for approved compatibility can complicate lift and sling purchasing as well as the boots-on-the-ground task of pairing lifts and slings in dynamic health care settings.
Cutting through the confusion starts by understanding sling types and materials, as well as the various ways in which they connect to lifts.
SLING TYPES, APPLICATIONS, & ATTACHMENTS
While patient sling design can vary from one manufacturer to the next, most slings fall into the following categories:
Seated slings. Used to transfer patients between wheelchair/recliner and bed.

- Turning, repositioning, and supine slings. Used for turning to the side, boosting to the head of bed, and positioning between prone and supine.

- Limb sling. Used to hold limbs
- Ambulation sling. Facilitates walking and help prevent falls.
- Sit-stand sling. Used for lifting up to standing with a powered sit-stand lift.

Slings can be made of fabric (synthetic or natural), mesh, or disposable materials. Also called single patient use, disposable slings are increasingly popular as facilities prioritize infection control. The difference between sling materials should directly inform laundering protocol, an important topic we’ll elaborate on below.
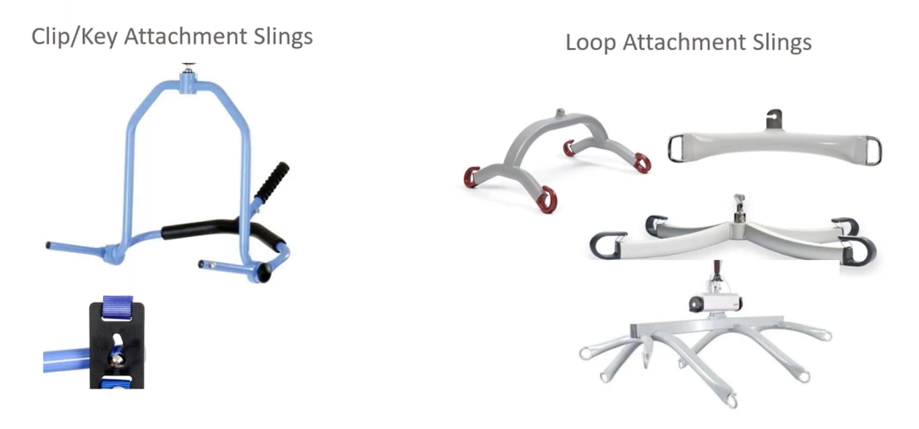
Hanger bar attachments can also differ between slings. Patient slings feature one of two attachment types: a loop attachment that slides onto and hangs from a piece of metal or a clip or key attachment that connects the sling to the hanger bar.

Hanger bar design must correspond with the attachment type. Loop attachments hang from pronged hanger bars. The number of prongs on a hanger can range from two to eight. Clip and key attachments, meanwhile, connect to hanger bars whose knobs feature compatible clips.
FACTORS TO CONSIDER IN SLING SELECTION
A helpful metaphor for sling selection: There are many types of shoes, but for marathon runners, running shoes are the only option. Any other footwear (tennis shoes, boots, sandals, flats, high heels) is likely to create risks and challenges or cause injury.
Similarly, choosing the right sling for a healthcare setting is key to preventing adverse events. Here are factors to consider when choosing slings:
- Clinical applications in continuum care. First and foremost, consider the sum total of healthcare disciplines that might need to use a given sling. If selecting slings for a nursing unit in a hospital or ambulatory setting, there’s a chance that the same sling might be used to transfer a patient to radiology, or to an oncology room. Give considerable thought to this possible range of use and let the sum total of possible uses inform sling selection.
- Sling size and weight capacity. Different sling manufacturers use different sizing systems and can have different weight capacities. For example, a size large sling from one manufacturer might have a weight capacity of 500 pounds – and might cap out there – whereas another manufacturer recommends a medium sling for a patient weighing 500 pounds. These differences underscore the importance of researching manufacturers to ensure that sizing aligns with your organization’s patient profiles. Ask yourself, “Will these slings hold our heaviest patients?” If more than one sizing system exists among your facility’s approved slings, ensure that staff is aware of and clear on any differing metrics and nomenclature.
- Sling service life and shelf life. Service life is the length of time during which a sling can be used once opened. A disposable sling might have a two-week service life; fabric slings can sometimes be used for years. Shelf life is the length of time that a sling can remain unopened before it is no longer cleared for use. When choosing slings and devising reordering timeless and related systems and processes, ensure that your organization’s use cycle and standard storage durations align with the sling’s service life and shelf life.
- Disinfection. All fabric and mesh slings require laundering. However, different sling manufacturers can have differing specifications for everything from wash and dry temperature to detergent compatibility (bleach, for example, can compromise the integrity of some fabric and mesh). Failure to abide by laundering guidelines can erode the integrity, and therefore the safety, of slings. Ask yourself when choosing slings: Is your laundry provider willing, capable of, and equipped to meet a manufacturer’s specific requirements for washing and drying slings on an ongoing basis? Disinfectant consideration is needed for wipeable slings, as well, as some are not approved for contact with bleach, which is common in wipes.
- Quantity available & replenishment. How many slings does a unit or facility need, how often will they need to be restocked, and how will units get more if needed? A process is essential. Note the word process – not person. When one individual is tasked with order and supply, problems can arise when that person is on vacation or absent unexpectedly. Sidestep such risk by putting teams and automated systems in place, ensuring that slings are in supply in any circumstance.
- Storage and accessibility. Where are you storing slings: in patient rooms, or somewhere else? Ideally, lift sling storage is close to the lift and to other related parts, such as lift batteries. Remember, the space where slings are stored must abide by manufacturer guidelines related to temperature, light, and any additional specifications. The matter of storage leads to the matter of accessibility. Is this sling storage spot a place where staff can access slings readily? Taking it one step further: If your facility uses slings with both loop attachments and clip and key attachments – are you storing slings in a way that easily distinguishes between the two, preventing busy staff from grabbing the wrong sling type?
- Maintenance for safe use. Do you have a procedure in place to report a defective or worn sling? If you use more than one sling, what safeguards exist to ensure that the correct sling is being used? What protocols exist to ensure that training and education are completed accurately, and in a timely manner?
KEY COMPONENTS OF SAFE SLING USE
Whether discussing sling-related incidents with colleagues or reviewing documented cases on MAUDE, some common themes and causes might emerge.
Incompatible slings and hangers is likely one of them. This issue, a leading cause of sling-related incidents, generally stems of lack of standardization within the same facility. This is a problem so prevalent and pressing that, in 2016, a group of safe patient handling and mobility experts formed a committee co-led by Lynda Enos and Lori Severson to investigate and address the matter. Their efforts resulted in an evidence-based document called the Healthcare Recipient Sling and Lift Hanger Bar Compatibility Guidelines. I urge healthcare professionals, facilities, and home caregivers to download this PDF and review and share its valuable contents, which go hand-in-hand with the Safe Patient Handling and Mobility Interprofessional National Standards Across the Care Continuum, published by the American Nursing Association and available for purchase here.
ESTABLISHING SYSTEMS FOR SLING-RELATED EDUCATION AND TRAINING
The resources above can help inform education and training. However, lift- and sling-related training is so important that we’re also offering some guidelines here, as well.
Hopefully a no-brainer: Healthcare providers who use slings need consistent, effective, and comprehensive training and education. This should not be one-time event. Training should occur at orientation, when an individual is hired, or when a new sling is introduced to the healthcare setting – whichever comes first. From there, training should repeat on an annual basis and any time there are changes to products or processes.
However, healthcare providers aren’t the only individuals who need to be well-versed in patient lifts and slings. The following stakeholders also need to understand slings – their mechanics, but also their value – because their buy-in has a huge bearing on sling-related safety and success organization-wide:
- Procurement teams. Procurement holds the purse strings and negotiates product contracts; they’re also the front line in ensuring manufacturer ISO compliance. Even more, procurement teams are likely to know which manufacturers offer quality products, related training, maintenance, and support, and abide by guidelines overall – a hugely valuable asset.
- Material management/supply chain teams. This team is critical to developing processes for stocking and storing slings, and therefore critical to ensuring that staff can readily access slings as needed. If your organization uses washable slings, these individuals can also interface with laundering teams to confirm process-related details, like where to put slings once they return from laundering.
- Department and unit leaders. It’s essential to involve these individuals in sling-related training for many reasons. Among them: they typically have a hand in staff training and are instrumental in holding staff accountable to the organization’s approach to slings and related lift equipment.
Education department. Last but certainly not least, keep your facility’s education department abreast of all matters sling-related. This is the team, after all, that will develop and coordinate training content that’s integral to proper maintenance and use.
Want more insights on ensuring safe sling use across your unit or organization? Earn one free contact hour by listening to the full on-demand webinar.
Yeu-Li Yeung, MS, OT/L, CPE, CSPHP

Yeu-Li Yeung, MS, OT/L, CPE, CSPHP, is a certified professional ergonomics, Certified Safe Patient Handling Professional, and a licensed occupational therapist with more than 20 years of experience in healthcare ergonomics.
Yeu-Li led the development and implementation of the Safe Patient Handling and Mobility (SPHM) Program at Duke University Hospitals and Clinics. Currently, she manages the SPHM Program with the Duke Nursing Executive Team. She also teaches SPHM at the Duke University’s School of Nursing and Occupational Therapy Doctorate (OTD) Program. Yeu-Li was instrumental in assisting the School of Nursing and OTD) Program in outfitting their simulation labs with SPHM equipment.
In addition, she provides cost-effective solutions to minimize work hazards in non-SPHM matters in the healthcare setting as well as ergonomic and SPHM recommendations to healthcare designs and renovation projects. Yeu-Li has presented on SPHM and ergonomics at national conferences, has published several articles on SPHM, and served on the Board of Directors for the Association of Safe Patient Handling Professionals.

